Columbia DIY Ventilator Challenge
Overview
We invite students, faculty, and staff from all Columbia schools, as well as external makers, inventors, and clinicians, to participate in the Columbia DIY Ventilator challenge. The goal of this challenge is to design a DIY (do-it-yourself) emergency ventilator. Specifically we are interested in a device that will inflate and deflate an Ambu-bag in a systematic manner, as an emergency stop-gap while critical patients are waiting for care that may not be immediately available. Experienced clinicians, engineers, and makers are also needed to advise teams and to help judge and improve entries.
Ventilators can help care for critical patients suffering from pulmonary diseases such as that induced by COVID19, where ventilator shortage is anticipated. For a review of some recent activity in this area, see Fortune Magazine’s article on Sprint to design thousands of ventilators.
Goal
The goal of this challenge is to design a device based on an Ambu-bag (Fig 1a) that can be used both for invasive ventilation (in hospital setting) and potentially for non-invasive ventilation using a mask. Ambu bags are standard common and low cost CPR devices that are typically used manually to perform resuscitation. See this CPR demo (minute 1:17) to see how an Ambu-bag is typically used manually.
In this challenge, we are seeking a design for a makeshift emergency ventilator that will squeeze this bag automatically at a specified amplitude and rate. This will be used to keep patients alive while they wait for a proper ventilator. The device can use something like an Arduino and a RC servo or stepper, and a simple user interface to set rate and amplitude. The device should be easy to fabricate so that many of these can be made quickly.
Scenario A: In-hospital forced periodic ventilation of intubated, sedated (or paralyzed) patients under medical care.
Scenario B: In-or-out of hospital assisted ventilation of alert patients using a face mask. For this scenario, the device must also include a sensor to detect and trigger beginning of air intake.
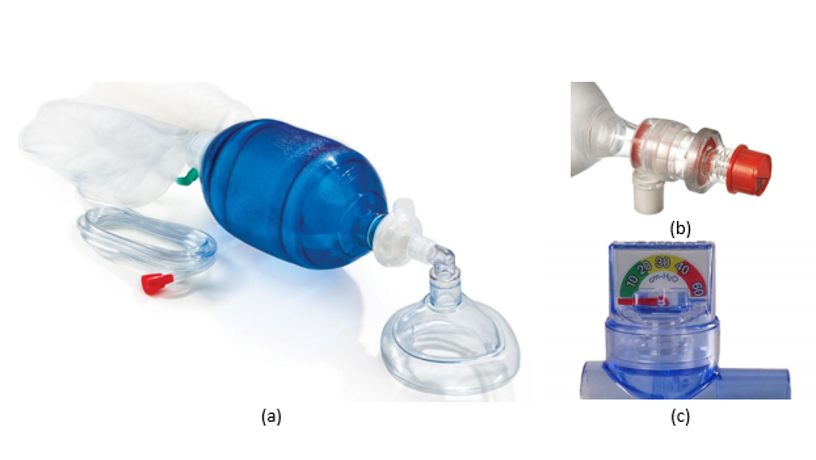
An Ambu-bag and regulator: (a) A typical Ambu-bag. Diameter of the blue bladder is approx. 6 inches. The requested device should squeeze and release the blue bladder by an adjustable amount and at an adjustable rate of 10-30 times per minute. (b) The bag is connected to a PEEP valve that passively maintains positive expiratory pressure on alveoli. (c) The device should be able to detect a sudden drop in pressure, for example by detecting the position of the arm on the analog manometer (c) or using a pressure sensor or position sensor external to the bag.
No physical construction or testing is required at this initial design stage. The inventors/designers retain all rights to their designs.
At the completion of the design stage, a team of experts will review the designs and offer up to $3,000 to each of up to 10 teams or individuals, to help prototype their designs. The reviewers will consist of product designers, engineers and clinicians.
Why DIY?
Commercial medical ICU ventilators are obviously preferred by clinicians and efforts are underway to manufacture and deliver more commercial ventilators, or even to make a single ventilator serve multiple patients. However, we are preparing for the eventuality that as a measure of last resort, people may need to make their own ventilators.
The DIY nature of the design must therefore allow anyone with basic engineering skills to procure components and assemble a working system from commonly accessible electrical and mechanical components and materials. Examples of common electrical components include Arduino and Raspberry Pi controllers, stepper motors, air pumps, batteries, pressure and airflow sensors, as well as common mechanical components such as bottles, pipes, tubes, bladders, fans, filters and valves. In addition, 3D printed and laser-cut plastic components can be used.
All software must be open source. Components and materials should be standard or Commercial-off-the-shelf (COTS) and as generic as possible. Single source components should be avoided if possible.
Out of hospital use of this device should only be done as a measure of last resort.
Problem Specification
The following are key requirements:
- The automated device will squeeze a standard ambu-bag by a specified amount (about 1 to 6 inches) and at a specified frequency (10 to 30 squeezes per minute).
- The squeezing mechanism can use an arm, a lever, a piston, a belt, etc.
- Maximum pressure in the bag is typically no more than up to about 30 cmH2O.
- The Ambu-bag has an attached PEEP regulator valve (Fig 1b) that the physician can use to set the minimum exhalation pressure.
- The attending physician will set the appropriate volume and rate to maintain reasonable lung pressure as determined using a manometer.
- The size of the ambu-bags can vary slightly, so the device should be compatible with (adjustable to) to accommodate a variety of bag sizes (diam 5-7 inches).
- The device should sit firmly on a base (e.g. a plywood base).
- Assume the ambu-bag is disposable. The bag should be easy to replace without dismantling the machine.
- The device should operate reliably and continuously for multiple days at a time.
- Ideally, the device should also detect a drop of pressure in the bag, and sound a loud audible alarm. A drop of pressure indicates a possible leak in the system, or a tube or mask being disconnected. The drop in pressure can be detected in many ways. For example, if the red needle of the manometer (Fig 1c) is at the lower end of the gauge, a small color sensor can attach to the manometer and detect the position of the needle. Alternatively, a pressure sensor can measure the pressure being applied by the bag to the base. Or a potentiometer can sense the position of the servo arm, or a current detector can measure how much torque is being applied by the servo. Anything inside the tubes that comes in contact with patient air must be either disposable or serializable.
- The units will connect to a power outlet with generator backup. No battery operation is needed.
- No need to worry about contamination. Viral filters, if needed and available, will be connected by the physician to the intake and exhaust tubes.
- No need to worry about oxygenation. If needed and available, oxygen line will be connected by the physician to the bag directly.
- There is no need for the device to be sterile or sterilizable.
- Materials should be standard and minimal. If you need to fabricate specialized components (e.g. using 3D printing or laser cutting), make sure that these parts can be fabricated quickly – avoid large or long prints and cuts.
Safety
- No human testing should be performed in the initial design phase. Any future testing on humans will require IRB.
- The device should be tested first on model lungs
- Critical sensors must be duplicate/redundant if possible
- System failure should result in an audible alarm (e.g. pressure drop due to tube disconnect)
- Students may not go on Columbia campus to fabricate the device
Challenge Timeline
Apr 2: Design Challenge Kickoff (Zoom webinar - noon-1pm) Click here to join the Zoom webinar
Apr 8: Contenders submit design proposals. See submission details below.
Apr 15: Selected teams receive budget (up to $3K) to build their design. This budget is intended to cover materials and components, tools (e.g. 3D printer) and other expenses. Contenders will receive the amount as a single sum and will place their own orders.
Apr 27: Video submission of final product and design
May 4: Selected winners announced. Winners receive additional funds after posting detailed instructions on Columbia DIY website
Submission Requirements
Submission format is a single PDF of a presentation (prepared in PowerPoint or Google Slides, for example) with the following information:
- Title slides: Rendering of complete design (including ambu bag), with names, affiliations, emails, and telephone of all participants. If a team submission, team lead should be identified and listed first. Separately list advisors and consultants who reviewed the design ore provided feedback.
- Additional CAD rendering, showing the entire system with all components labeled clearly. CAD must include everything, including base, ambu-bag, all fasteners, belts, wires, sensors, and electronics components. Link to an animation video is a plus.
- Basic specifications, including min max rate (pumps per min), maximum force that can be applied to the bag, amplitude range (minimum and maximum stroke length at the bag), list of sensed conditions and safety measures, number of parts, total cost of parts, list of tools needed for construction, estimated number of hours for construction.
- Full parts list, with link to purchase source, and cost (assuming small quantity purchase).
- Caveats: List of known issues with this design, that would need to be addressed in the future, or features that were omitted by design as a tradeoff decision.
- Requested funding. May include components, parts, tools, and services. Please give a rough estimate. List any other available sources of funding.
- References and acknowledgements: List all sources (with links) that you used or that inspired your design. List also papers and any other resources that you used. Acknowledge any help, sponsorship, advice or input you received from anyone other than those listed on the title page. Disclose any conflicts of interests.
- Please label your PDF 'LastName_ColumbiaVentilatorChallenge'. Submissions are due by 11:59pm on Wednesday, April 8.
Related Work
There are various open source ventilators already designed published. Feel free to learn from those, improve and combine existing designs and ideas. Please cite references and sources.
https://www.kare11.com/embeds/video/89-6dec725a-ed19-48c6-87e0-0c4c6cd9e3ba/iframe?jwsource=cl
Advisors Needed: Clinicians, Engineers, and Designers
If you are a practicing clinician, engineer, or experienced maker, and would like to help answer technical questions or guide teams, we would be glad to receive your help! Please join the Slack Channel below to comment and answer questions.
If you are interested in helping judge the final contributions, or have any other comments on this challenge, please contact the organizers directly.
Resources and Costs
- Ambu bag: https://www.amazon.com/gp/product/B086669DBM
- Model lungs for testing :
- Pressure sensor: https://www.amazon.com/Adafruit-Square-Force-Sensitive-Resistor-FSR/dp/B00SK694YE
- Arduino, etc: Adafruit, Amazon
- Servo set with feedback (17Kg-cm): https://www.amazon.com/Hiwonder-LX-16A-Robotic-Controller-Control/dp/B073XY5NT1
Order your own materials and components and keep receipts. All reasonable material and component expenses used in the process of designing and testing this system will be reimbursed.
Teaming and Submission
Participants are encouraged to use Slack Channel to find potential teammates, and to discuss technical questions.
Submit to: [email protected]
Challenge Lead: Hod Lipson, Columbia University
Advising Clinician: Nicos Hadjiangelis MD, NY Presbyterian Brooklyn Methodist Hospital